First of two parts
Illnesses are a part of childhood, but nothing could have prepared these mothers for the time when their children, just babies at the time, were diagnosed with an illness that they would carry with them for the rest of their lives.
In October 2017, Joanne Valencia noticed that her three-year-old daughter, Sophia, was drinking a lot of water and sleeping all the time. Joanne thought that Sophia was just building healthy habits when she started school.
But in the months that followed, Joanne noticed her daughter rapidly losing weight and wetting the bed. By December, Sophia had high fevers and breathing problems that were no different from her usual asthma attacks. He also had a hard time waking up.
It took three visits to different hospitals for them to get a proper diagnosis, and by then, Sophia had already been in a coma for about 24 hours.
At the third hospital, the nurse told Joanne, “‘Mom, just my suggestion, let’s ask for a urinalysis and get a sugar test.’ (“Mom, I suggest you ask for a urinalysis and we do a blood sugar test.”)
That’s how they knew Sophia has type 1 diabetes (T1D).
Diabetes is a chronic condition that occurs when the pancreas produces little or no insulin or the body does not use insulin properly. Insulin is necessary for glucose, a type of sugar, to be absorbed into cells to provide energy.
While type 2 diabetes (T2D) is the most common disease that is characterized by insulin resistance and is often associated with high sugar intake, T1D is diabetes. autoimmune disease where the body mistakenly attacks and destroys the beta cells of the pancreas that produce insulin.
Sophia’s glucose rose to a life-threatening level of 600 milligrams per deciliter. A normal blood sugar level it will be around 70 to 140 mg/dL.
He was already in a state of diabetic ketoacidosis (DKA) which is caused by too much glucose and not enough insulin, which caused him to lose consciousness.
A similar tragic event happened to Jennifer Linga and her son, Neo, who was two years old when he was diagnosed with T1D in 2020.
“On the first ER (emergency room) visit…he was misdiagnosed with asthma,” Jennifer shared. “We were advised to use a nebulizer at home. But as a mother, your instincts are different.” (We were advised to nebulize at home. But as a mother, your instincts are different.)
Neo received the correct diagnosis at the second hospital they visited, when he was already suffering from DKA with a glucose level of 500 mg/dL. He was in a diabetic coma for more than two days.
“For me as a parent, it was very scary…. It numbs your heart and your mind because you don’t know,” Jennifer said.
T1D is usually seen in children, but it can be diagnosed at any age. The risk of developing it is higher in people with a family history of diabetes, but both mothers said they had no history of the disease.
“In fact, family history (as a risk factor) of type 2 diabetes is much higher,” said Dr. Lorna Abad, a pediatrician at the Philippine General Hospital. (In fact, family history as a risk factor is high for type 2 diabetes.)
“If you have that (unique) gene (that will make you diabetic), you will have it. In fact, the antibodies … that destroy the beta cells of the pancreas, they found in the test that there are babies when they are born, who already have that immunity,” he added.
(If you have that variant gene that makes you diabetic, you will have it. In fact, research has found that some babies are already born with that special antibody that destroys the beta cells of the pancreas.)
Jennifer feared for her son’s life. “(His) life is just beginning, then suddenly he will be told that he needs daily injections, constant monitoring of blood sugar, and … constant visits to the hospital.”
(His life was just beginning, and then suddenly he was told that he needed daily injections, regular blood sugar monitoring, and regular hospital visits.)
Misdiagnosis trends
T1D is much more common than T2D, affecting only about 5% to 10% of diabetics. There is no known cure for it.
T1D does not show any symptoms in its early stages, but it can become severe within weeks to months. Some of its symptoms include frequent urination, increased thirst and hunger, sudden weight loss, fatigue, abdominal pain, and DKA.
Because T1D shares symptoms similar to other diseases, the risk of misdiagnosis or delayed diagnosis is high.
As the co-founder of Type 1 Diabetes PH Parents, Jennifer said many children in her community were misdiagnosed because doctors often did not order blood sugar tests and instead diagnosed pneumonia, asthma or other diseases with similar symptoms.
“It is necessary here that the level of suspicion is high, because about 40 percent of children with type 1 diabetes when they go to the hospital, it seems (the situation) is bad… because the initial indicators of a child having diabetes are not recognized,” Dr. Abad said.
(The level of suspicion should be high. 40 percent of children with type 1 diabetes arrive at the hospital in a critical condition, because early signs of diabetes were not recognized.)
The doctor stressed the importance of educating parents and guardians to recognize when a child is drinking alcohol and urinating excessively can indicate early diabetes.
Healthcare providers are no exception. “Of course, among primary health care providers, they should also be aware. The history will always be asked, even if the complaint is (just) a cough, like that…. We have what is called a system review, so everything (of the medical history) is reviewed,” he added.
(Of course, primary care providers should also be aware. Always ask about the history, even if the complaint was just a cough. We have what we call a system review that reviews the patient’s entire medical history.)
Common misconceptions
Lack of awareness leads to common misconceptions about T1D.
“I feel because there is discrimination when it comes to T1 and T2,” Joanne said. “He has an umbrella inside one as if they don’t accept that they are two different things…. (People think) that it is a situation that you have caused yourself.”
(I feel there is discrimination when it comes to T1 and T2. They are lumped together as if people don’t realize they are two different things. People think it’s self-inflicted.)
Dr. Abad emphasized that what children eat is not related to developing T1D, unlike T2D, which can be acquired through poor diet and lifestyle.
With T1D, “You can’t (prevent) pancreatic damage” (you can’t prevent the pancreas from getting damaged), the doctor explained.
It’s also not true that children with T1D can’t eat and live normally, as Sophia and Neo are still allowed to have candy – but with an insulin dose already. Sophia is also a runner at school, while Neo currently enjoys cycling and motorcycling.
“We want to give her the most normal life she can have, even with this condition,” Joanne said of her daughter.
Neo’s mother, Jennifer also said: “The resilience of children (with) T1D is amazing (The resilience of children with T1D is amazing). They can do (many things) by themselves.”
The daily life of a child with T1D
Today, Sophia, who is now 12 years old, and Neo, who is eight years old, are thriving under their parents’ care, which includes a strict daily routine.
Both children wake up at 5 to 6 a.m. to have their glucose levels checked, then they are injected with the appropriate dose of basal insulin to keep their blood sugar stable throughout the day. Before meals, they give bolus insulin to control the rise in sugar from food intake.

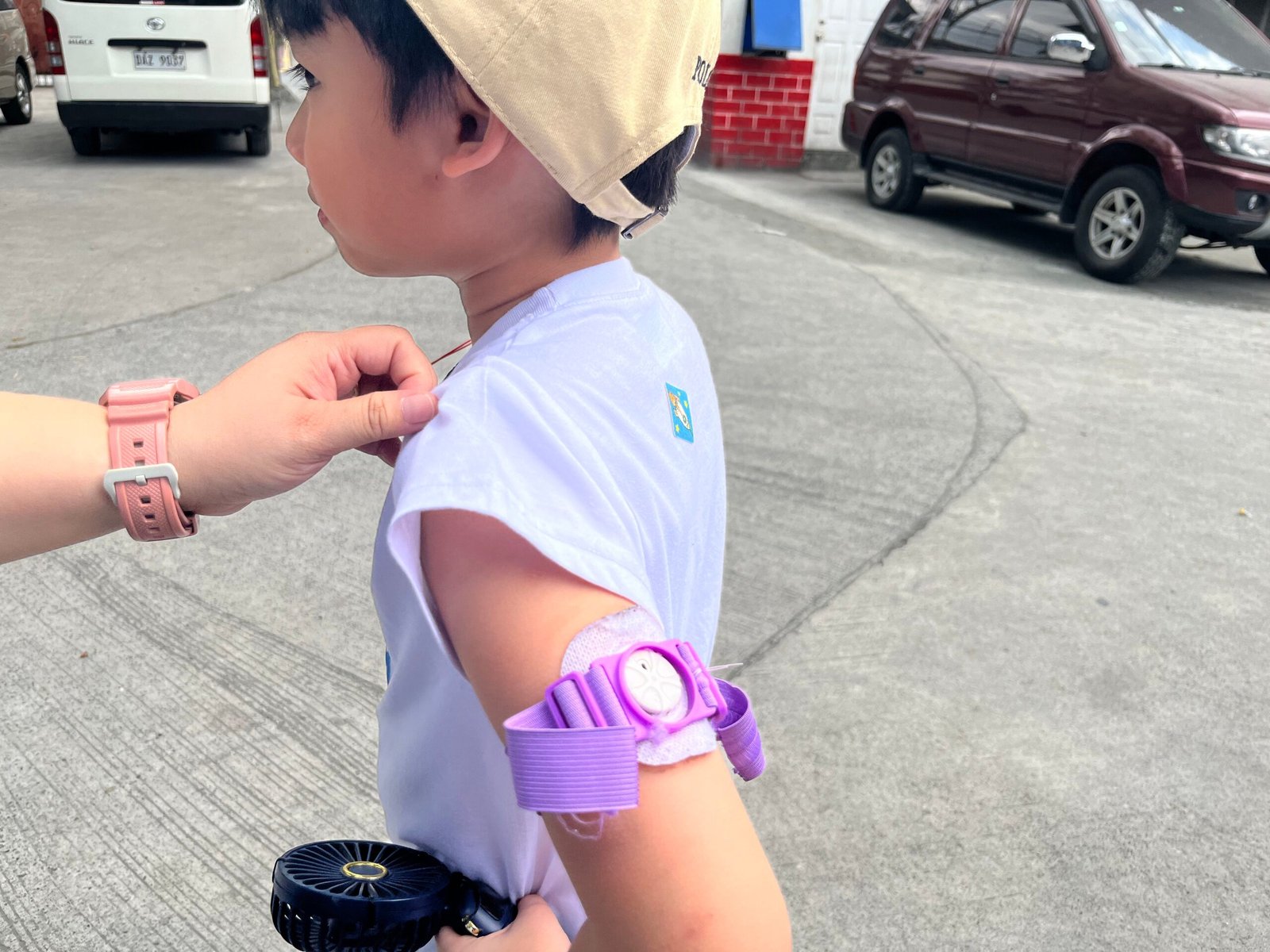
When they sleep, their parents still have to check their blood sugar through a continuous glucose monitor through a sensor worn on the children’s wrists.
For children aged six to 12glucose levels should be between 70 and 120 mg/dL before meals and at bedtime, and less than 140 mg/dL one to two hours after a meal.
Meals are usually portioned, with meat and vegetables taking up the majority of the plate. Children can also be given a small portion of dessert.
“Whatever he eats, we also eat…. That seems to have become the norm at home,” Jennifer shared an event. (Whatever he eats, we eat too. That has become our routine at home.)
Dr. Abad supported this practice, saying that the whole family should have the same diet to control not only their children’s sugar, but also everyone else’s.
Parents as ‘living pancreas’
Managing a condition like T1D is difficult, but Sophia and Neo’s parents accepted the responsibility once their children were diagnosed years ago.
“It’s a condition that requires 24/7 attention,” Joanne said. “Since Sophia was diagnosed, our lives can no longer be lived by choice. Every day (requires) planning and making decisions. Because otherwise (Because if not), it won’t work.
Jennifer said: “At the moment he has no news what happens to him (about what happens to him)…. You will be the one to inject, you will be the one to know his current blood sugar – because right now, you are his living pancreas (because right now, you are his living pancreas).” – Rappler.com