Gentle, painful and inhuman. This is how Angie List describes her mother’s recent death.
“It was a mixture of sadness and relief that he passed,” List says.
“But he shouldn’t have suffered like he did.”
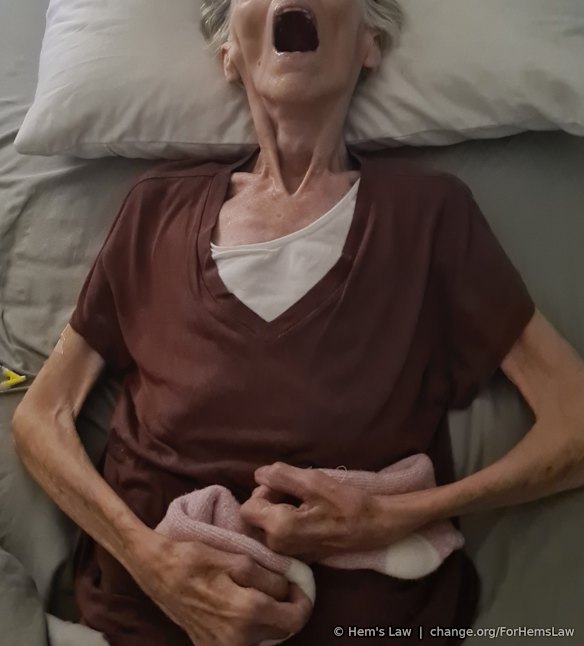
Warning: This story contains a poignant depiction of Helen Lister in the weeks before her death.

At the time of her death, List’s 79-year-old mother – Helen Lister – weighed 24 kg. For more than 10 days, her mouth was stagnant, inside cracked and dry.
He had lost the ability to swallow and was slow hunger – late sign Alzheimer’s diseasewhich he was discovered in 2023.
List helped her parents move into an Ascot house following the diagnosis.
But attempts to comfort her mother there in her final weeks – hydromorphone for pain and sedatives to reduce agitation – were thwarted by pressure ulcers that developed on her weakened body.
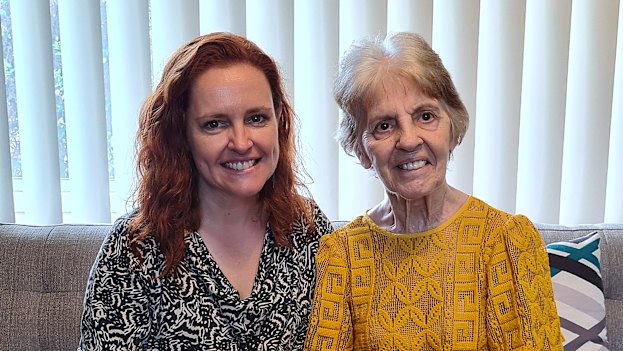
“The respite care staff was wonderful, and they were caring,” List says.
“But I knew (pain sedation) wasn’t 100 percent effective because when we tried to gently put him back … he would go into shock.”
List’s experience of watching his mother slowly die from dysphagia and cachexia, the medical terms for swallowing disorders and wasting, was inspired. campaign wanting the establishment of the “Hem Law”. (“Hem” is the nickname his mother used instead of “Bibi”.)
Such legal provision – which will be different discretionary aided legislation – will allow a family member or legal representative to “choose a peaceful and humane death on behalf of a person with dementia” under a set of specific criteria.
“This is not a judgment of quality of life, it is a judgment of quality of death,” List says.
“It’s not a decision about whether or not to end a life. It’s a decision about whether the death will be long and painful for all involved, or whether the death can be compassionate and quick.”
Helen Lister was brought up in rural NSW, an upbringing that her daughter says shaped the calmness she carried through her life.
“He had an incredible warmth and instinct for knowing what people needed,” List says.
“He was endlessly resourceful, creative and kind.”
His calling was many and varied, starting from running a hair salon and catering business; to help her jockey husband, Arthur Listermanaging a horse stud, later writing a book about his racing career; writing a column for the local newspaper, teaching at TAFE and running charity drives.

“He loved fun … he had business cards called ‘Lister’s Fun House’ with his and his father’s names listed as directors,” List says.
“Changes in his ability to plan” was one of them the first signs of decreased recognition of Hem. He spoke to his doctor, who referred him for further investigation.
Eight months later, in September 2023, Lister was diagnosed with Alzheimer’s disease.

Alzheimer’s is the most common type of mental disorderaccounting for nearly 70 percent of the investigation, according to Alzheimer’s Research Australia.
The list says a lack of education about the progression of the disease, especially in the advanced stages, is a driving force behind its campaign.
“Before this happened, I had no idea how deadly dementia and Alzheimer’s disease are,” he says.
“I’ve always been confused as to how someone dies… I didn’t really understand that it’s the brain and body connection that’s broken, (creating) neurological challenges.”
What Hem’s Law asks:
A unique legal provision – unlike existing assisted dying legislation – which allows a family member or legal representative to choose a peaceful and humane death on behalf of a person with dementia, but only when all of the following are independently verified:
- Loss of swallowing, confirmed by a doctor or speech therapist
- A live dying phase approved by two independent doctors, confirming that palliative care is the only option left.
- Written confirmation by the decision maker, and an independent legal and medical witness
People in late stages of dementia gradually losing the ability to walk, communicate, eat, drink and swallow. As the body becomes weaker, it struggles to fight infections and diseases, with pneumonia being the most common cause of death.
Research shows dysphagia – dysphagia – is a “highly associated disease of Alzheimer’s”, estimated to affect 84 percent to 93 percent of patients in the moderate to severe category.
“This is not dangerous. In the last stage of dementia, it is a relapse,” List says.
“The brain systematically destroys the parts of the cortex that coordinate swallowing. Once it’s gone, it doesn’t come back. This is the mechanism by which dementia kills.”
List says the possibility of cachexia has also been obscured by discussion of the condition.

“Insanity is now leading cause of death in Australia … people have to say that when it gets to a certain point (they can make end-of-life wishes).
“But if we don’t tell people what the end is, should they say what option they want?”
Neurologist Professor Peter Nestor, associate professor of neuroscience at the university Queensland Brain Institute and the Mater Hospital, is concerned that too much information during early diagnosis can be overwhelming for patients.
“If you were to (provide) every situation (of death) that could happen, you would end up beating people,” Nestor says.
“And generally, in my clinical experience, I find that people (diagnosed with dementia) don’t want to know about the end at the beginning.”
Dementia progresses differently among patients, he says. As with the deteriorating schedule, it is difficult to tell people “exactly what their last few days will be like”.
Need to improve knowledge of death around dementia has been raised in other circles, with some advocates of voluntary assisted dying calling for the law to include neurodegenerative conditions.
Under current legislation, people living with dementia in all Australian jurisdictions have excluded from receiving a VADfor two main reasons: circumstances affect the ability to make decisions, and the length of time people have to live is different. Some people live for decades after diagnosis, others, like Lister, a few years.
Ben White, professor in life law and regulation at QUT, says expanding VAD to include dementia is important but presents complex challenges, and any changes to the law should be based on Australian evidence.
“That should include it attitudes of people living with dementia,” he says.
“Certainly if Queensland, or anywhere else, were to go through the an example of an advanced requestby definition, you will need to be informed clearly and carefully about the possible ways, in order to make information (the end of lifedecisions).

List maintains that Hem’s Law should exist separately from the VAD law, and says a version of what it recommends is already happening in mild settings.
“Decisions about levels of sedation, about the pace of comfort care, about what constitutes ‘adequate’ symptom control – these are made every day, behind closed doors, by individual clinicians acting out of conscience and compassion, with no legal protection for themselves or their families,” he says.
“Hem’s Law brings nothing new. It replaces the medical lottery with a legal right.”
About an hour into the conversation about his mother, a memory from List’s early 20s floats up.
The time had come to put down the family’s 19-year-old dog, who at the time was suffering from arthritis and could not walk.
“Mom said, ‘the time has come’, and I said, ‘How do you know?’,” List recalls.
He replied: “I can tell by his eyes, by the way he looked at me.”
“I knew that my mother would have wanted that too. The fact that I could not give it to her made me very sad.
“If (Hem’s Law) is his legacy, what he leaves for the world, I know that would make him happy.”
Start the day with a summary of the day’s most important and interesting stories, analysis and insights. Sign up for our Morning Edition newsletter.




